Tags
Harborview Medical Center, Julie Lary, Motorcycle injury, Rajalary, Rich Lary, scribbles writing
My second day in ICU was focused on getting me ready to move to acute care. I needed to pass several medical milestones, including taking x-rays to confirm the correct placement of the Erector Set in my left leg, assessing the stability of my vitals and health, and establishing whether I could stand up with the help of a walker.
The nursing staff works 12-hour days, usually 2 to 3 days per week. For each shift change, the assigned nurse and assistant come into your room, introduce themselves, then write their name on a white board. Also, on the white board are notes about medications, procedures, and expectations, such as “sit-up” and “use walker.”
Michael (I think that was his name) was my assigned nurse on Wednesday, my second day in ICU. He was quirky, and upbeat. I was so happy when he came into my room because of his effervescent personality. The day before, feeling nauseous, I was given a small, plastic “barf” pan, which I named Barfy. For two days, I held onto that pan, as if it was a stuffed animal, squishing it when I felt anxious or in pain, and rotating it around when bored.
Michael shared in my adoration of “Barfy,” recognizing the inanimate object provided comfort.
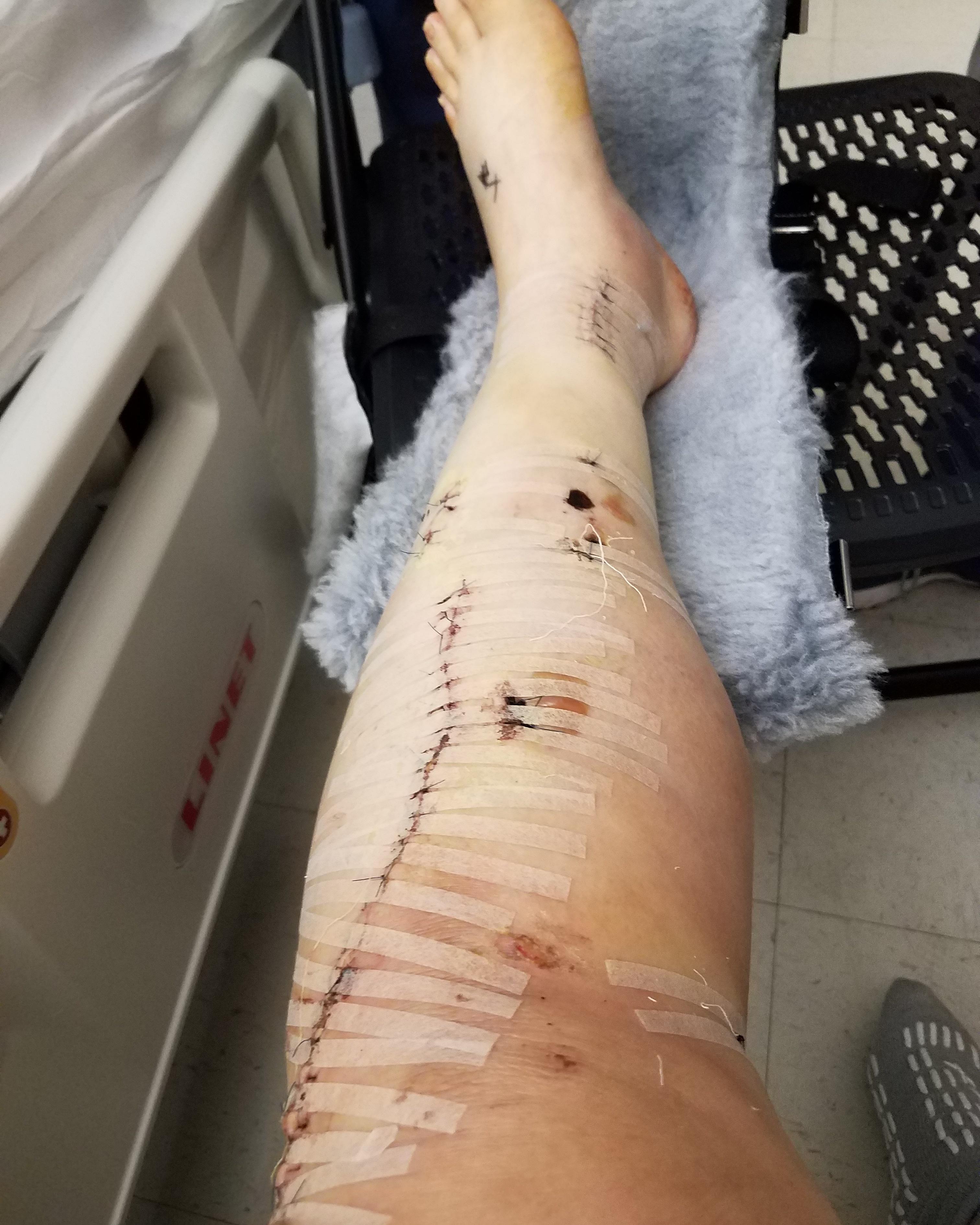
Very early in the morning, two members of the orthopedic team visited to examine my left leg. Throughout my stay, they came every morning, removed the ace bandages and gauze, took pictures of the wounds (evidently part of my tibia broke through the skin), and tested the leg’s flexibility and pulse – marked with an “x” on the top of the foot. They provided the reassurance I needed to push through the pain.
An hour or so later, a physician and several medical students, visited my room, some appeared genuinely interested, others indifferent. They didn’t stay long, mainly because I wasn’t a very interesting case: An older woman with a rebuilt leg.
Shortly afterwards, a somber group shuffled into my room, an older man in a crumpled shirt with dated brown plaid tie and brown polyester slacks, and two young women who reluctantly came into the room. The man identified himself as a psychiatrist, sharing they were conducting a study and wanted to know my interest in participating.
Called “A Comparative Effectiveness Trial of an Information Technology Enhanced Peer-Integrated Collaborative Care Intervention for US Trauma Case systems (Trauma Survivors Outcomes and Support),” the study entailed a new treatment to help people overcome physical and emotional concerns following a serious trauma. Depending on a participant’s needs, they’d provide a peer who’d recovered from a serious injury, nurses, doctors, social workers, and other health care providers.
The study felt very wishy-washy with no definitive treatment plans besides, “We’ll provide the necessary resources to help you recover.” Over the course of several days, they visited several times to validate my interest in the study. The two women, however made me feel more insecure than confident. On the day they were supposed to screen me for the study, one of the women walked in, and a moment later dashed out, saying she needed to be elsewhere. A few minutes later, the second woman appeared and was able to conduct the 45-minute survey to determine my eligibility.
While I’m sure the questions were baselines for comparing responses in subsequent months, they were repetitive and biased towards getting a positive response in the future. I had to grit my teeth as I repeatedly said, “significantly worse” to questions like “Do you have less interest in doing activities since your accident?” They also asked, “Do you have difficulties climbing stairs” and “Do you have difficulties doing everyday activities like getting dressed?”
“Ahh… I’m lying in a hospital bed with multiple fractures and can’t even pee by myself. What do you think?”
A day later, they said I wasn’t selected to receive the extra care, but would still be included in the study. While I’m glad I don’t have to bother with additional meetings and calls with care providers, I can guarantee with 100% certainty, the control group (people like me) won’t emotionally recover as quickly as those who receive extra care. Duh!
More importantly, how can you compare one trauma survivor to another? Someone who’s bed- or wheelchair-ridden for months is going to have a slower recovery than someone who can return to their normal daily activities within a few weeks.
Roomies for a few days
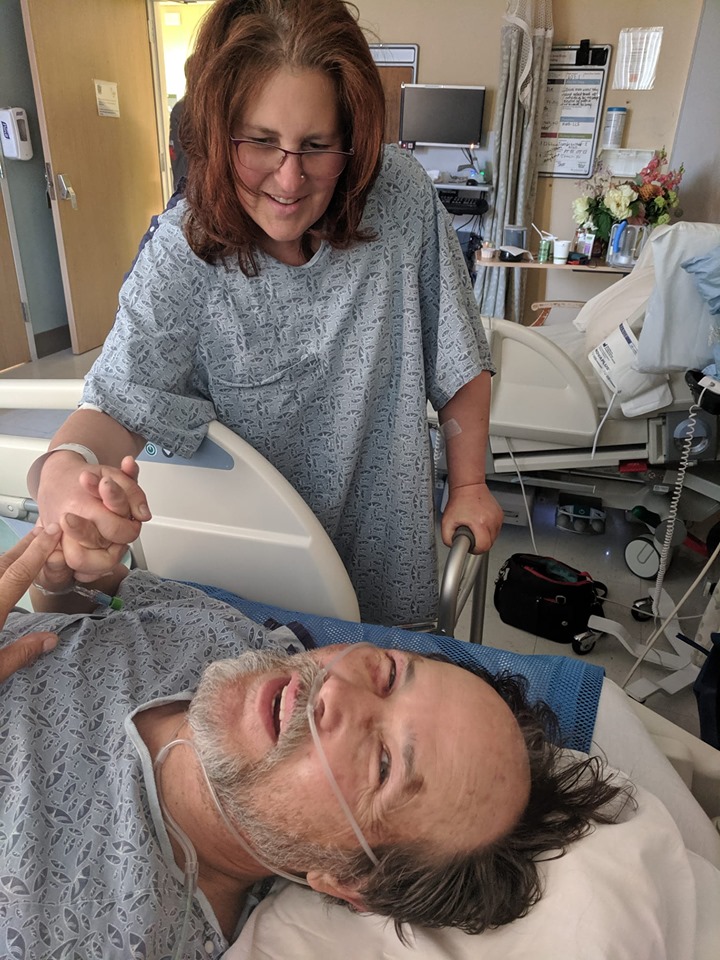
Around noon, Stacey wheeled Rich into my room. It was the first time I’d seen him since the accident. He looked like a boxer who’d just finished 12 rounds, draped in a white blanket with a black eye and scrapes on his face, groggy, and obviously more interested in climbing back into bed then being wheeled down the hallway.
My eyes went straight to his legs. His right leg rested on the foot of the wheelchair. His amputated leg stuck out uncomfortably, no knee, no calf, just a gauze-wrapped stump.
My heart sunk as I feigned delight in seeing him. I’m not sure he was fully aware of what had occurred or that I was also in the hospital. I can’t remember what we said or even if we spoke. Our meeting was less than 5 minutes.
In the afternoon, two physical therapists dropped by. While I desperately wanted to get out of bed, and knew what to expect, it came as a surprise when sitting up made me dizzy. My heart was pounding, and my blood pressure skyrocketed. After a few minutes of resting, I was able to stand on one leg, and hold onto a walker, but it was obvious I couldn’t take more than a tiny hop.
The therapists laid me back down and raised the foot of the bed to help my blood flow. I laid like that for the rest of the day, completely zonked, floating in-and-out of sleep.
At the end of the day, I was disconnected from IVs and monitors, and what few personal items I had were assembled so I could move to a regular hospital room. We took the elevator down a floor or two, and then wheeled by the nurses’ station. One of the nurses exclaimed, “She’s going to be with her husband,” then put her hand over her mouth, realizing she’d wrecked the surprise.
However, I already knew Stacey had worked with the hospital to get us in the same room. No doubt, as soon as I saw Rich, my spirits lifted. We could talk and see each other, and when no one was watching, I could use my walker to hop over to his bed and absorb his calm demeanor.
Teflon Man
The oldest of four children, Rich was always more independent, industrious, and introspective. At Christmas, he’d open his gifts, bring them to his room, and play with them by himself. He was the one who helped make dinner, care for his younger siblings, and was assigned more time-consuming chores like painting the fence and kitchen.
Complementing these qualities is his extraordinary calm demeanor and rational (rather than emotional) approach to life. His ability to see the positive and work through whatever life throws at him, earned him the nickname “Teflon man.”
Indeed, he doesn’t get phased by little things and takes the big stuff – like the amputation of his left leg – into stride.
I’m the opposite. The little stuff is worrisome and the big stuff mammoth, and anything that goes wrong is cause to fret, cry or scream.
Two defining days
When I was wheeled into the acute care room, I was not only delighted to see Rich, but a huge bouquet of amazing flowers, including a beehive ginger, pink anthurium, white peonies, pink columbine, coral snapdragons, green hydrangea, and an array of unusual greenery. Not only was the bouquet spectacular, but fragrant.
Several times a day, I would get complements on the bouquet, including a nurse, who helped me identify the flowers by downloading to my phone PlantSnap.
My amazing employer Bridge Partners Consulting sent me the bouquet, which brightened my days in the hospital, rehabilitation center, and when I got home.
That evening, my fabulous, always upbeat manager Jessica Harbin, visited, bringing me a coloring book and pencils. More importantly, she eased my mind. With Microsoft’s fiscal year ending in June, I was working on several “rush” projects, and felt horrible that I couldn’t complete them. Plus, as a contractor, I was scared that I wouldn’t have a job after coming home.
I was told, not to worry. She’d find me work whether I wanted to work part- or full-time. Did I mention Bridge Partners is an amazing company that truly cares about its employees?
The following day, Thursday was a bit stressful. Rich had his initial amputation early Tuesday morning, probably after the operating rooms were freed up after the rush of patients on Memorial Day. On Wednesday evening, he couldn’t eat or drink anything. Thursday morning, he was hungry and thirsty, plus his throat hurt from the breathing tube he had earlier.


Parched, hungry, and uncomfortable, he had to patiently wait until he was taken away for his second operation, which more thoroughly closed the amputation wound, and added extra tissue at the bottom so it would be less painful when he gets a prosthesis.
Happily, the surgery wasn’t very long, and by late afternoon, he was wheeled back into the room. While dopey from anesthesia and hooked up to a plethora of monitoring equipment and IV pumps to infuse gabapentin, to deaden nerve and phantom pain, he was in good shape with strong vitals. I breathed a sigh of relief.
Meanwhile, my energy level hadn’t improved, and my heart rate and blood pressure were widely fluctuating. A quick test later, and the physicians had the answer. I was anemic. While I was slightly anemic when I arrived at Harborview, my red blood cell count had plummeted in the subsequent days.
I hadn’t put two-and-two together. Not only had I lost blood when the accident occurred and during surgery, but the blood cell-producing marrow in my left thigh had been replaced with a metal rod. My body was struggling to produce enough red blood cells, leaving me weak and tired.
I hadn’t realized getting a blood transfusion was a big deal. Two nurses must double-check and sign-off on the paperwork, and I also had to sign a release form, indicating I realized the risk of getting a blood transfusion. After all the ”t’s” were crossed and “i’s” dotted, a bag of red blood cells was slowly dripped into my veins over several hours.
Before the IV could be started, the nurse had to call in some resources. After having IVs in my arms for several days, the veins in my arms had collapsed. The inside of my left arm had turned purple and there wasn’t a vein in sight. A stat nurse was called to evaluate my veins and remaining IVs, one of which he felt could be used for the transfusion.
Later in the day, a medical professional used a venous ultrasound to find an untampered vein and start a new IV. I felt badly because I’d asked to have two IVs removed when I was in ICU. It never occurred to me that I would need them in the future for a transfusion!
Just when Rich was starting to recover from his second amputation surgery, several physicians arrived to say they were going to do a cerebral angiogram on Rich on Friday because they spotted an aneurysm on his CT scan, performed a few days earlier. The non-invasive procedure examines the internal blood flow and performance of vessels and arteries in the head and neck.
Poor Rich was back to fasting, and even though they said the procedure would be done first thing in the morning, he wasn’t whisked away until close to noon for the procedure. The entire time, he wanted to eat or drink something, and continued to complain about his throat hurting.
I was glad when he finally left, knowing he’d be back in a few hours. However, when he returned, he was very agitated and within minutes, a woman walked in with some machine, and placed a headband on Rich’s head to validate something or other. Rich was supposed to stay still for 20 minutes during the test, but he kept fidgeting and moving, complaining about seeing strange dots and flashes of light.
The more the technician asked Rich to stay still, the more he squirmed. She grew obviously frustrated with him. There was nothing I could do since I was still too tired to get out of bed. I implored him to stay still, but it was like talking to the wall.
Happily, Stacey and Chris showed up to placate him, and explain since he’d had an angiogram, where dye was injected through the femoral arteries near his groin, he had to lie flat and still for several hours to prevent bleeding. They feed him ice chips until he was cleared to sit up and eat. Stacey ordered him mashed potatoes, which he said tasted awful, exacerbating his frustration and agitation.
Late that evening, a young woman physician arrived to share the results of the angiogram. Rich had two aneurysms, the one at the top of his head, just over his eyes, was disturbing and had the potential to burst at any time. The other aneurysm was smaller at the back of his head with a low probability of rupture.
Bluntly, the physician explained Rich would need to undergo brain surgery on Monday to “clip” the aneurysm. My heart dropped.
While the idea of clipping the aneurysm “sounded good” because it meant it wouldn’t rupture, leading to instant death or irreparable damage, it meant more surgery. Brain surgery. And as I wrote previously, modern medicine is like a movie, they only reveal what you need to know at the moment, not all the details.
Of course, we all agreed to the surgery, believing it’d be over in a few hours.
To be continued…
